Common Ticks of Virginia
ID
2906-1396 (ENTO-487NP)
Introduction
Multiple species of ticks are commonly found in Virginia, but not all species are found in all areas. Not all ticks are infected with pathogens that cause disease.
American Dog Tick
The American dog tick, Dermacentor variabilis, measures about 5 mm long and has short, stout mouthparts. It is dark brown with a white shield on the adult female or light wavy lines on the adult male (Fig. 1). It is found mostly in the western regions of Virginia and west of the Blue Ridge Mountains. Adults are most commonly found.

Figure 1. American dog ticks. Adult female, adult male, nymph, and larva (CDC).
Lone Star Tick
The lone star tick, Amblyomma americanum, measures about 5 mm or less in length. It is light reddish-brown with a small central white spot on the back of the adult females, and several white markings on the back of the adult males (Fig. 2). The immature “seed ticks” stages do not have these markings. All stages have reddish-brown legs. The lone star tick can be very common in the Piedmont and Coastal Plain regions of Virginia.
Deer Tick
The deer tick, Ixodes scapularis, is a small tick measuring about 2-3 mm in length. The mouthparts are long and the legs are dark colored (Fig. 3). The body appears off-white or reddish when fully fed. The deer tick is also known as the blacklegged tick.
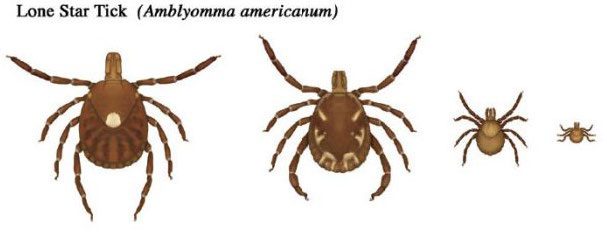
Figure 2. Lone star ticks. Adult female, adult male, nymph, and larva (CDC).
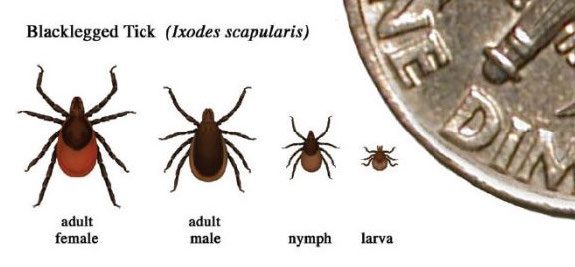
Figure 3. Deer or blacklegged ticks. Adult female, adult male, nymph, and larva (CDC).
Asian Longhorned Tick
The Asian longhorned tick, Haemaphysalis longicornis, was recently found in Virginia in 2018. It is a smaller tick, measuring 2-3 mm long, with short, squat mouthparts (Fig. 4). The body is reddish-brown without any white markings on it. The US populations reproduce asexually, allowing populations to build up in localized areas. The Asian longhorned tick is largely found in the western half of Virginia, along the Blue Ridge Mountains, and in the northern part of the state.

Figure 4. Adult Asian longhorned tick (Eric Day, Virginia Tech, Bugwood.org).
Tick Removal
Ticks are best removed with tweezers or by wrapping the tick in a tissue and pulling it out with fingers. Grasp the tick as close as possible to the skin and pull slowly with even pressure to avoid leaving the mouthparts in the wound. Do not twist or jerk as this will leave the mouthparts in the skin. Do not use nail polish, petroleum jelly, alcohol, or hot matches to remove the tick. Wash the wound with an antiseptic after the tick is removed. Kill the tick in rubbing alcohol and keep it in a small vial for a few months in case any disease symptoms develop and the tick needs to be identified.
How to Avoid Ticks
The following methods of prevention are recommended by the Virginia Department of Health.
- Avoid tick infested areas such as tall grass and dense vegetation.
- Walk in the center of trails and avoid brushing against weeds and tall grass.
- Keep grass and underbrush mowed and thinned.
- Wear light-colored clothing so ticks can be easily seen.
- Tuck pant legs into socks so ticks stay on the outside of pants.
- Conduct tick checks on children and pets every four hours when staying outside.
- Apply insect repellents containing active ingredients such as DEET, picaridin, oil of eucalyptus, Bio-UD, or IR3535 to exposed skin.
- Ask your veterinarian to recommend tick controls for your pets.
- Treat your lawn with an approved pesticide for tick control.
- Treat clothes with permethrin following all label precautions.
Ticks and Diseases
Consult a medical professional for any questions regarding suspected tick-transmitted diseases. The following list does not include all the potential diseases transmitted by ticks in Virginia. Avoiding tick bites is the best way to protect yourself from tick-borne diseases.
Rocky Mountain Spotted Fever (RMSF): A tick must be attached for 4-6 hours to transmit RMSF to its human host. The first noticed symptoms are usually severe headache, chills, fever, muscle aches, nausea, vomiting, and other flu-like symptoms usually starting 2-14 days after the tick bite. By the third day after the bite, a red rash develops on the wrists and ankles in most cases, and may spread over the body. A blood test is needed to confirm the disease and antibiotics should begin early if RMSF is suspected. American dog ticks and lone star ticks transmit RMSF.
Lyme Disease: Lyme disease is rarely transmitted in the first 24 hours of tick attachment, so frequent checking and prompt removal of any ticks is strongly recommended. Lyme disease initially develops as a rounded, red ringed “bulls-eye” rash, usually 2 or more inches in size at the site of the tick bite. The rash may not be well-defined in appearance and is seen only in 70% of Lyme patients, who still develop flu-like symptoms such as nausea, headache, fever, and general stiffness of the neck joints. A small percentage of untreated people develop chronic symptoms of arthritis and nervous system complications. Lyme disease can only be confirmed by a medical doctor with specialized laboratory tests. Deer ticks transmit Lyme disease.
Ehrlichiosis, Anaplasmosis, and Babesiosis: These tick-borne diseases have symptoms that include headache, fatigue, and muscle aches. Symptoms usually occur within 1-2 weeks following a bite by an infected tick. Diagnosis requires specialized laboratory tests administered by a medicalprofessional. Lone star ticks transmit ehrlichiosis, and deer ticks carry anaplasmosis and babesiosis.
Alpha-gal Syndrome (AGS): AGS, also known as red meat allergy, is a potentially life-threatening reaction to the alpha-galactose (alpha-gal) sugar molecule found in the meat of non-primate mammals. Lone star ticks carry the alpha-gal sugar in their saliva, and it is thought that a bite from a lone star tick may trigger the body’s reaction to the presence of alpha-gal sugar in red meat. Alpha-gal can also be found in milk, gelatin, meat extracts, and similar by-products. Symptoms of AGS include hives, itching, swelling of the face and throat, shortness of breath, and intestinal upset. Reactions often occur several hours or more after exposure to alpha-gal. AGS is a food allergy that may develop into anaphylactic shock requiring emergency medical treatment in some individuals.
Some species of ticks can also transmit various viral diseases, such as Heartland and Powassan. Lone star ticks are associated with Southern Tick-Associated Rash Illness (STARI), which is similar to and may be mistaken for Lyme disease. Asian longhorned tick carries several human diseases outside of the US, but pathogens have not been detected in US populations to date.
Additional Resources
CDC, Alpha-gal Syndrome. https://www.cdc.gov/ticks/alpha-gal/. Accessed 8 December 2021.
CDC, Anaplasmosis. https://www.cdc.gov/anaplasmosis/. Accessed 8 December 2021.
CDC, Babesiosis. https://www.cdc.gov/parasites/babesiosis/. Accessed 8 December 2021.
CDC, Ehrlichiosis. https://www.cdc.gov/ehrlichiosis/. Accessed 8 December 2021.
Virginia Department of Health. Ticks and Tick-borne Diseases of Virginia. https://www.vdh.virginia.gov/content/uploads/sites/12/2019/08/Tick-borne-Disease-in-Virginia-Flyer-8.5-x-11-format-for-website-.pdf. Accessed 8 December 2021.
Revision
Revised by Theresa A. Dellinger, December 8, 2021.
Virginia Cooperative Extension materials are available for public use, reprint, or citation without further permission, provided the use includes credit to the author and to Virginia Cooperative Extension, Virginia Tech, and Virginia State University.
Virginia Cooperative Extension is a partnership of Virginia Tech, Virginia State University, the U.S. Department of Agriculture (USDA), and local governments, and is an equal opportunity employer. For the full non-discrimination statement, please visit ext.vt.edu/accessibility.
Publication Date
January 30, 2022



